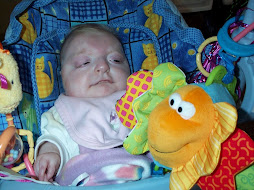
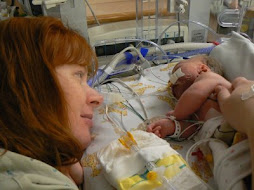
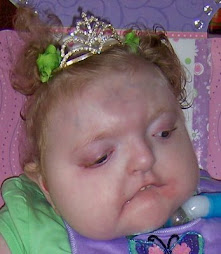
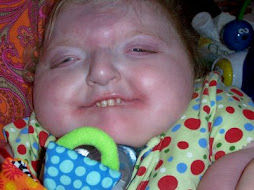
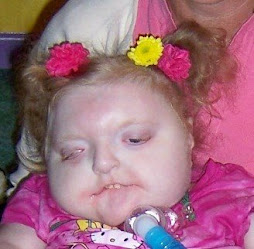
Darling Brosie has been doing very well since being home. He continues to be down on his O2 needs. He is active and playful and back to his usual tricks of partying all night, much to my dismay.
Sunday, February 21, 2010
Tuesday, February 16, 2010
HOME at last!
I am writing this from home sweet home with a snoozing Ambrose on my lap.
Since we left the hospital he is down on his O2 need and down on his pressure support.
He must be happy to be home!
Sunday, February 14, 2010
Hard day for Daddy
 Brosie' home ventilator: The Pulmonetics 1150
Brosie' home ventilator: The Pulmonetics 1150
Crazy days-
Yesterday Ambrose's Daddy got in a car accident. He was banged up quite a bit but lucky to have not been injured seriously. His truck however is totaled.
Ambrose is doing better and on track for his planned homecoming on Tuesday.
He is adjusting to his ventilator. I think he was having some plugging issues. No one ever listens to me when I tell them that he needs higher than normal temperature settings on his humidification. They wait until he starts to dry out and have troubles. The pulmonologist was in agreement with me on that and since it has been turned up, his secretions have thinned and he has stopped having desats. He has also come down some on his O2. I have learned that the frequency and size of his breath changes the amount of O2 his is receiving.
I also wanted to mention that he has his flexion/extension CT scan a few days ago. As predicted, it showed a very abnormal C-spine with narrowing at the base of the skull, but they felt it did no look unstable. Interestingly it also revealed that he has an ear infection. (10 days of fevers, multiple labs, negative for everything and no one looked in his ears.)
On a happy note: Ambrose's Mommy received an acceptance letter from Vermont Technical College for their nursing program.
Friday, February 12, 2010
What's wrong Brosie?
Not sure what is going on but Ambrose is again having a difficult day.
He has been on his home vent since Thurs afternoon. Seemed to adjust to it just fine.
Then he started needing more O2 (up to 4L from 1L) to keep his sats up and was quite agitated. He sounds pretty clear. They took an Xray and it looked pretty much the same. Scoped his trach - looks fine. He had a low grade fever. Got some Tylenol and settled down but continued needing more O2. They also increased his pressure support from 5 to 8. They are not sure what the problem is and say it may be just him adjusting to the different vent but I'm not sure I buy that.
Thursday, February 11, 2010
Wednesday, February 10, 2010
GRRR!
...Well that did not go so well. I had to fight to get heard by a Dr. who seemed annoyed by my questions. He put in a cuffed trach which is 2 whole sizes bigger than his regular uncuffed trach. I fought back tears as it caused him to bleed. I do not want to have to do this to him myself and on a weekly basis. (also it can possible harm his trachea, is uncomfortable to him, is torturous to put in, and seems to take away his voice.) They are assuming that he will continue to need a cuffed trach although he did not have one before, he has an acute illness and he is getting better. No one has really explained to me the reason for this assumption. I have been aware that he could potentially need one if he were to use pressure support at home. But he is not on pressure support. So perhaps he will not need it for long but they did not seem to want to explore what the options would be even though he would likely require a custom trach which takes weeks to order.
Also the Dr. who wants to manage his home vent usage has not been communicating with me. The other Dr. who was willing to do so has been checking in on us frequently.
The medical supply co. respiratory therapist worked hard to get a vent available to us quickly and it will be brought here sometime tomorrow for him to get used to and me to get training on. Unfortunately we can not go home until Tuesday as that is when she is available to come set it up in our home, train us and the local branch's resp. therapist. I don't think he really needs to be here that long but I am glad we actually have an end point in sight. Being here is a huge upheaval to all of our lives. I want to get him out of here before he picks up any hospital bugs.
It's 4:15 pm. I had trouble sleeping thinking of ?s I wanted to ask the ENT Dr. who was supposed to come yesterday. I came in at 8:00 a.m. because I didn't want to miss him. I am still waiting.
The most annoying thing is I he was in the PICU several hours ago to see another patient.
Gotta go. He's here.
Tuesday, February 9, 2010
Today has been a bit frustrating although Ambrose is doing well, Thankfully!
I have been persuing getting a home ventilator for Ambrose since we have been here. It was brought up in the past when he needed CPAP but we wound up opting for getting CPAP through a different system. He weaned off of it but we continued to use it at night preventatively. When he was sick we used it all of the time. One of the problems is that it is not portable. I didn't want to take him off of it to go to the Dr. Also, it is not actually delivering the amount of PEEP it is supposed to because we do not have the high flow it needs to work properly. Additionally with the occasional episodes that he has had where he required some bagging, I feel that the ability to give him some pressure support would be a good thing. It seems that everyone was in agreement about it and I was trying to prevent his discharge from being held up because no one initiated the process of ordering this equipment and arranging for training me, etc. I've been asking about it for a full week. Today, after really pushing it has only just now been ordered. I'm told it can take a week unless they actually had one in stock, which I won't know until tomorrow. So frustrated! We need to get home and he is doing much better.
An additional issue that needs to be figured out is his trach. His anatomy is so unusual that standard trach tubes often don't sit right in his trachea and can occlude causing him distress. The reason is not always apparent to those around him who wind up giving him additional support that he may not need when the problem may be simply: airway.
He has been using a custom trach that is longer and has a sharper curve than usual. The ventilator has a problem with the air leak around that trach, so he needed to have a cuffed trach put in. It is hard to get in and causes bleeding. The cuff is inflated so there is no air leak, allowing the ventilator to work more efficiently. Of course, it is not custom made for him, so there are issues as mentioned previously. One being that he seems to need an unusually high amount of air in the cuff. There have been a few times he has seemed to be gasping through his mouth which shouldn't happen when you have a trach. The solution had been to go up to a bigger size. Now they are talking about a bigger size yet. I'm not sure if he is going to need this for home. I really don't want to have to force a large cuffed trach into him, causing him to bleed. They ordered a custom cuffed trach but it takes weeks to get and they've changed size since then anyway. I'm waiting for the ENT Dr to come scope his trach again. Of course he is looking through it when he is in a perfect position, not necessarily how it looks as he is moving throughout his day.
Right now he is off on an expedition to get a flexion/extension CT scan to look at his C-spine.
Monday, February 8, 2010
Freak fever
I had to run home today. When I left Ambrose was looking good. Then I got a call that he had a 102.5 fever. They took a new set of cultures and switched antibiotics. When I returned he was once again looking good. No more fevers. What was that all about?
Sunday, February 7, 2010
Ambrose had a very good day!
Today darling Ambrose came off pressure support and didn't even seem to notice. He's been back down to 35% on his O2 and alert and playful all day. Daddy and Grandma and Grandpa came to visit. He had one episode that needed some bagging but it seems to be related to coughing, secretions, and trach position.
Keep up the good work Brosie!
7 in Heaven
Saturday, February 6, 2010
Saturday was a quiet day/I saw the bunny
Not much happened today. Ambrose was up a bit on his O2 but seemed more like himself. No fevers, improvement in color and quantity of trach secretions. His blood culture came back in the middle of the night growing something but they think it was just a contaminated sample, since an earlier culture was clean and he's not having any symptoms. Of course they drew another one just to be safe and decided to put in an IV even though 2 attendings said he didn't have to have one. But of course now that it's there they won't remove it. Ambrose seems to be working on that himself. Our friend and Ambrose's early interventionist, Mary came to visit us and brought some treats and a bag my husband put together for us as well.
I was just speaking with the mother of a 1 year old with leukemia and the mother of a 3 1/2 year old with neuroblastoma cancer who just had his 9th surgery. We were speaking of how amazing and loving and HAPPY our children are! (Not to mention Brave. When you are afraid to do something, just think of them.)
As a complete aside - I saw the bunny today. Two years ago, when Ambrose was born and I spent the whole cold winter here with him in the ICN, there was a black rabbit who lived outside of the North entrance of the hospital. People would leave lettuce and apples and the like in the snow. When I saw the bunny I knew it would be a good day.
"Bunny Rabbit" was a nickname I had for Sophia and it felt like a little sign from her. One day it practically came running up to me, as if she said," hurry, there she is!"
I later learned that the previous summer someone had released some domesticated rabbits there because they thought the patients would enjoy watching them out the windows. (There are some patient rooms right there at ground level.)
As I've approached the hospital these past several cold mornings I wondered if the rabbit (or rabbits) was still around. When I saw him this morning it just made me so happy!
Friday, February 5, 2010
Bigger trach = Better results
The ENT doc just came and changed his 4.0 PED cuffed trach to a 4.5 and, despite some bleeding, he is ventilating better and able to come off of the rate and back to his previous settings of just CPAP and pressure support (7 over 8). Mechanical problem indeed. Thank God!
Ambrose is having a BAD morning!
When I came in this morning Ambrose was on pressure control with a rate of 24 on the ventilator. (Meaning he is no longer breathing on his own with just the extra pressure of CPAP and Pressure support.) Apparently he started having some severe desturation episodes where his sats were as low as 20 and not going much over 60 with bagging. He has had several doses of xopenex (avariation of albuterol with a different propellent) and duo nebs. He had 2 less severe episodes yesterday that responded to the bagging and xopenex.
His blood gas showed high potassium and CO2 but when they rechecked them from a venus sample they were OK.
He had another fever. (Day 8)
PICU attending Dr. Braga's careful observation led him to notice that there was a problem with his trach. (Ambrose has very unusual anatomy and currently uses a custom trach that is longer than usual with an increased angle because the standard sizes tip back and occlude against the back wall of his trachea and also to try to bypass areas of tracheomalacia. When they put him on the vent originally for just the CPAP and pressure support it would not work due to the significant air leak around his usual (uncuffed) trach. They needed to put in a cuffed trach which is a standard pediatric size. The larger diameter of the cuffed trach made it difficult to put in and resulted in blood tinged secretions for the first 2 days.) He noticed that Ambrose was breathing through his mouth. When he moved the trach around a bit he seemed to do better. So they over inflated the cuff , which may be holding it in a better position for him and he seemed to be breathing much better. They subsequently were able to decrease some of his vent settings, but he is still on a rate and higher pressure support than yesterday. So we are hoping this is more of a mechanical issue than a worsening of his lung disease. We are waiting for his ENT Dr Smith to come scope him and give his guidance about what trach may be best. (They ordered a custom cuffed trach for him but it will take a few weeks.)
Please send strength our way.
Thursday, February 4, 2010
Positive Pressure is a "+"/A+
Ambrose remains stable. No big changes. He continues on pressure support of 7 over PEEP of 8 at 35% O2. The good news is that is chest xray looks good - no pneumonia, relatively clear. Without those distractions however it is very noticeable how crooked his spine is and that his heart is really far to the left. (He is definately NOT a republican.) He continued having scattered fevers (but none so far today). They decided to start him on antibiotics last night based on the continued fevers. (Last night was day 6 of fever.) He is getting Cipro and Tobramycin nebs. His trach grew moraxcella. (sp?) Virus panels were all negative. (Which doesn't mean he doesn't have a virus but they only test for a few major ones.) He still has tons of secretions, but they are no longer blood tinged from the trauma of having a cuffed trach put in. He seems more comfortable to me.
His Daddy visited yesterday and brought some of Ambrose's little buddies, including "Little Buddy" (Thank you Ben) and "Pierre the Polar Bear" (Thank you Carole!) "Marvin," and "Spotty." They were all happy to see each other.
Today he will be getting some physical therapy. Yeah!
Brosie is such a good boy!
Wednesday, February 3, 2010
Ambrose in PICU 2010


 My darling Ambrose has been sick along with Mommy for the last 5 days. The first few days he had fevers of up to 102.9, lots of coughing and increased discolored secretions. The good news was that he was NOT requiring any more O2 than usual. I kept him on his CPAP around the clock for additional support. Tuesday morning, after moving him, he couldn't keep his sats up despite cranking his O2 up as far as it goes (10L). Similar to previous episodes, he required bagging. (He is breathing but need some extra force behind his breaths to get in enough O2.) He would sat well with bagging him at 10L, but we can not do this continually. So we called rescue, transported him to BMH where they bagged him for over 2 hrs. until the DART team came to transport him to DHMC's PICU. They put in a cuffed trach because he had a big air leak around his trach. The cuffed trachs are hard to get in and cause some bleeding. Ouch!
My darling Ambrose has been sick along with Mommy for the last 5 days. The first few days he had fevers of up to 102.9, lots of coughing and increased discolored secretions. The good news was that he was NOT requiring any more O2 than usual. I kept him on his CPAP around the clock for additional support. Tuesday morning, after moving him, he couldn't keep his sats up despite cranking his O2 up as far as it goes (10L). Similar to previous episodes, he required bagging. (He is breathing but need some extra force behind his breaths to get in enough O2.) He would sat well with bagging him at 10L, but we can not do this continually. So we called rescue, transported him to BMH where they bagged him for over 2 hrs. until the DART team came to transport him to DHMC's PICU. They put in a cuffed trach because he had a big air leak around his trach. The cuffed trachs are hard to get in and cause some bleeding. Ouch!He is getting pressure support (basically the same thing as bagging but controlled by a machine) and CPAP through the ventilator. He is stable. Don't think he'll be here long but you can never predict.
Subscribe to:
Posts (Atom)